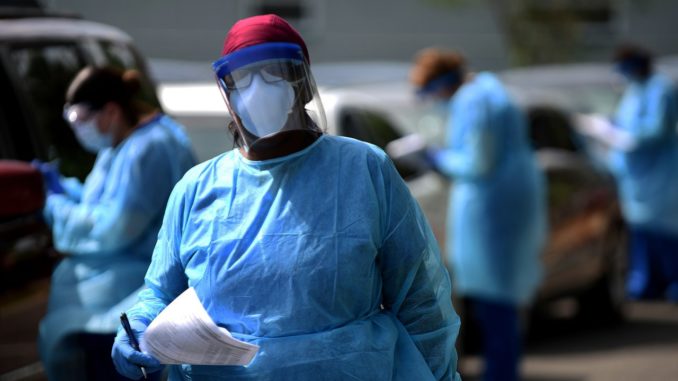
The National Black Nurses Association and Direct Relief identified five Covid-19 hotspots in need of PPE and other supplies.
By Talya Meyers
When New Orleans became a Covid-19 hotspot, C.J. Marbley’s small 50-bed hospital quickly filled. At the pandemic’s peak, New Orleans East Hospital was treating 57 Covid patients, said Marbley, the hospital’s chief nursing officer. At one point, a nurse who worked in the intensive care unit became sick and then died of the disease. Her death shook the hospital’s staff.
“Her coworkers were taking care of her along with taking care of other ICU patients,” Marbley said. “It hit home.”
Marbley was concerned for his patients, comprised primarily of African American and Vietnamese community members.
“We recognize the magnitude of the health disparities in our communities compared to the rest of New Orleans and the rest of the nation,” he explained. “When these pandemics hit, the ground is fertile for very bad outcomes.”
New Orleans East Hospital, like health care providers around the country, ran low on personal protective equipment – Marbley compared it to a gas light coming on – but never went without.
Still, the hospital lacked the PPE supply needed to offer mobile testing and education — interventions that Marbley considered essential.
A lot of Marbley’s patients are service workers, he explained. “They’re not in jobs where they could work at home,” he said. “They need to know not only how to take care of themselves, but what their status is…so they can protect their families and their coworkers.”
But then he heard from an organization where he was a member, the National Black Nurses Association. They had found a reliable source of PPE – enough to supply five different Covid-19 hotspots with the supplies they needed.
That source was Direct Relief.

THE NATIONAL BLACK NURSES ASSOCIATION
NBNA, founded in 1971, has 114 chapters across the U.S. The organization does everything from providing education and professionalization opportunities to members to publishing a peer-reviewed journal.
Fundamentally, “the mission for the National Black Nurses’ Association is to make sure that African Americans and other communities of color are getting the best possible access to care,” said Millicent Gorham, the organization’s executive director.
That means, in part, equipping the nurses who serve communities of color that have been disproportionately affected by the virus. “We’re very keen about the nurses being frontline providers. They’re the ones who are seeing the Covid patients most often, so they need to be protected,” Gorham said.
As the Covid-19 pandemic gained ground, NBNA began working with Team Love, a philanthropic organization started by the musician, entrepreneur, and activist Sean “Diddy” Combs. Combs hosted an online dance-a-thon designed to raise money to help communities of color fight against Covid-19.
The money – approximately $4 million – was given to Direct Relief to help organizations like NBNA.
“We wanted to make sure black and brown communities were given the help that they need,” explained LaToya Marc, vice president of strategy and operations for Combs Enterprises.
NBNA, which she described as a “grassroots” organization with chapters around the country, “is able to speak to the different needs” in individual communities.
Badly needed around the U.S. in “hotspots” – areas with high incidences of Covid-19 – was PPE like N95 masks and gloves, along with hand sanitizer, pulse oximeters, thermometers, and other supplies. Direct Relief and the NBNA worked to identify five locations, each strongly represented by communities of color, to receive these supplies.
For Gorham, it’s particularly meaningful that members of the NBNA are able to bring these supplies directly to their communities. Oftentimes, it’s hospital administrators who make decisions about what’s acquired and how it’s distributed, she said.

ENGAGING COMMUNITIES
Debra Toney, one of the designated recipients, is a member of NBNA and the vice president of quality management at Nevada Health Centers, Nevada’s largest Federally Qualified Health Center. The donation of PPE to her health center, she told Direct Relief, will help her and her colleagues continue serving “those patients who are living in impoverished neighborhoods where there’s a lack of services.”
“Getting PPE is a mess out here,” she said. “It’s a daily scavenger hunt, trying to make sure you have enough equipment.”
While Nevada Health Centers has switched some of its services to telehealth, Toney said that some patients have conditions that require them to be seen in person – or they simply don’t have the digital resources required for a telehealth visit. “People still show up. You just have to be prepared,” she said.
For Toney, having the health center’s doors open to serve patients is a personal mission.
“I consider myself a community activist…who happens to be a nurse, and community engagement is huge,” she said. “Patients depend on health care professionals to provide them with the education and guidance they need.”
For Marbley, a mobile testing unit – impossible without the donated supplies – is a way to protect his patients and the larger community from Covid-19. But it’s also a way to engage communities.
Many of New Orleans East Hospital’s patients aren’t aware of what resources are available to them, he said. Some are also afraid to come to the hospital, which means that existing conditions are at risk of going untreated. The mobile unit is a way for staff members to connect with the very people who most need care.
“It provides an extra opportunity to get into these communities, not only to test them, but to link them to care, link them to education,” Marbley said.
Direct Relief, since sending its first Covid-19 response shipment on January 24, has granted more than $27 million in emergency funding and delivered more than 11,000 shipments of medicine and supplies to health centers and clinics in underserved communities across the U.S., including more than 4.5 million masks (N95 and surgical), 2 million gloves, 77,000 gowns and coveralls.






Be the first to comment